Why even non-drinkers are at risk—and what we can do about it
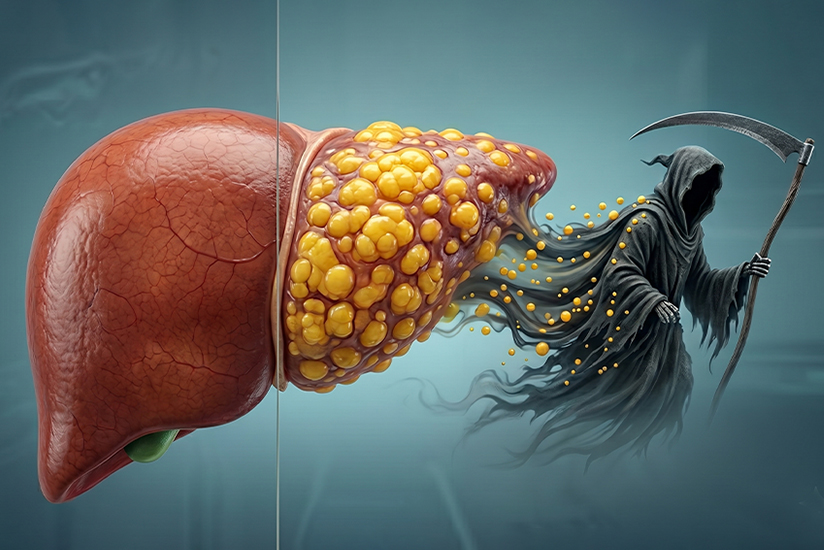
For many Filipinos, liver disease is still associated with alcohol. But a quieter, more insidious condition is rapidly rising across the country—fatty liver disease, now increasingly seen even in those who rarely or never drink. Driven by modern diets, sedentary lifestyles, and metabolic disorders, this condition often progresses silently for years before revealing itself as cirrhosis, liver failure, or even cancer. The most alarming truth? Many people who have it feel completely well.
By Rafael R. Castillo, MD
A Disease You Don’t Feel—Until It’s Advanced
Fatty liver disease, now more accurately termed metabolic dysfunction–associated steatotic liver disease (MASLD), occurs when excess fat accumulates in liver cells.
In its early stages, there are: no pain, no clear symptoms, no warning signs.
Yet beneath the surface, the liver may already be undergoing: inflammation, cellular injury, progressive scarring (fibrosis). And left unchecked, this can lead to cirrhosis, liver failure, or hepatocellular carcinoma.
Why Filipinos Are at Increasing Risk
The rise of fatty liver disease in the Philippines mirrors rapid lifestyle changes.
Diet Shift
- High rice consumption
- Sugary beverages
- Processed foods
- Low fiber intake
Sedentary Lifestyle
- Office-based work
- Increased screen time
- Reduced physical activity
Metabolic Conditions
- Obesity
- Diabetes
- Hypertension
- Dyslipidemia
Even individuals who appear “not overweight” may develop fatty liver due to visceral fat accumulation—a common pattern in Asians.
The Spectrum of Disease
Fatty liver disease exists along a continuum:
- Simple Fatty Liver (Steatosis)
– Fat accumulation without inflammation - Steatohepatitis (MASH/NASH)
– Fat + inflammation + liver injury - Fibrosis
– Progressive scarring - Cirrhosis
– Advanced, irreversible damage - Liver Cancer
– Potential end-stage complication
Clinical Importance: More Than Just the Liver
Fatty liver disease is not just a liver problem—it is a metabolic disease.
It significantly increases the risk of:
- Heart disease (leading cause of death in these patients)
- Stroke
- Kidney disease
- Type 2 diabetes progression
How Is It Diagnosed?
Fatty liver is often discovered incidentally during:
- Routine blood tests (elevated ALT/AST)
- Ultrasound imaging
- CT scan or MRI
More advanced evaluation may include:
- FibroScan (liver stiffness measurement)
- Non-invasive fibrosis scores
- Liver biopsy (in select cases)
Can It Be Reversed? Yes—If Caught Early
One of the most hopeful aspects of fatty liver disease is that it is potentially reversible in early stages.
Nutrition
- Reduce sugar and refined carbohydrates
- Increase vegetables and fiber
- Limit processed foods
Physical Activity
- At least 150 minutes/week
- Even modest weight loss (5–10%) improves liver health
Weight Management
- Reduce visceral fat
- Focus on waistline, not just weight
Control Comorbidities
- Diabetes
- Hypertension
- Lipid disorders
The Filipino Opportunity: Prevention at Scale
The Philippines is at a critical crossroads.
As urbanization and lifestyle changes accelerate, fatty liver disease may become one of the leading drivers of:
- Liver failure
- Cancer burden
- Healthcare costs
But unlike many diseases, fatty liver is largely preventable.
A Shift in Mindset
We must move away from this belief: “Basta hindi umiinom, safe ang atay.” (So long as we don’t drink alcohol, liver is safe.)
Toward this truth: “Diet, weight, and lifestyle now matter just as much—if not more.”
Final Message
Fatty liver disease is a silent epidemic—but it does not have to become a silent tragedy.
The earlier we recognize it,
the earlier we act,
the greater the chance we reverse it.
Because in liver health, as in many things in life—
what we do quietly today
determines what happens loudly tomorrow.
“Fatty liver disease is a silent condition with loud consequences—by the time symptoms appear, the damage may already be advanced.”
References
- Younossi ZM, et al. Global epidemiology of NAFLD/MASLD. Nat Rev Gastroenterol Hepatol. 2018. doi:10.1038/nrgastro.2017.109
- Rinella ME, et al. AASLD Practice Guidance for NAFLD. Hepatology. 2023. doi:10.1002/hep.32810
- Eslam M, et al. Redefining fatty liver disease (MASLD). Lancet Gastroenterol Hepatol. 2020. doi:10.1016/S2468-1253(19)30368-3
- Chalasani N, et al. Diagnosis and management of NAFLD. Hepatology. 2018. doi:10.1002/hep.29367
- World Health Organization. Obesity and metabolic disease reports. 2024
- Asian Pacific Association for the Study of the Liver (APASL). NAFLD guidelines. 2022
- Department of Health (Philippines). NCD Prevention Program
- Philippine Statistics Authority. Leading causes of mortality
Feature: Diet Plan for Fatty Liver Patients
Healing the Liver Through Everyday Food

A liver-friendly diet is not complicated—it is consistent.
What to Eat More Of
Leafy vegetables (malunggay, kangkong, pechay)
Fruits (papaya, apple, berries)
Whole grains (brown rice, oats)
Legumes (monggo, lentils)
Fish (especially omega-3 rich like bangus, sardines)
What to Reduce
Sugary drinks (soft drinks, milk tea)
White rice in excess
Processed meats (hotdogs, tocino)
Fried foods
Alcohol (if present)
Sample Filipino Plate
- ½ plate vegetables
- ¼ lean protein (fish/chicken)
- ¼ brown rice
Key Principle
“The liver heals when the diet simplifies.”
Patient Handout (Clinic-Ready)
Fatty Liver: What You Need to Know

What is it?
Fat buildup in the liver not caused by alcohol.
Why does it matter?
Can lead to cirrhosis and liver cancer.
What can you do?
Lose 5–10% of body weight
Exercise 30 minutes daily
Eat less sugar and processed food
Control diabetes and cholesterol
When to see a doctor?
- Abnormal liver tests
- Diabetes or obesity
- Family history of liver disease
Good news:
Early fatty liver can be reversed.
CME Brief
Fatty Liver Disease (MASLD) in Clinical Practice
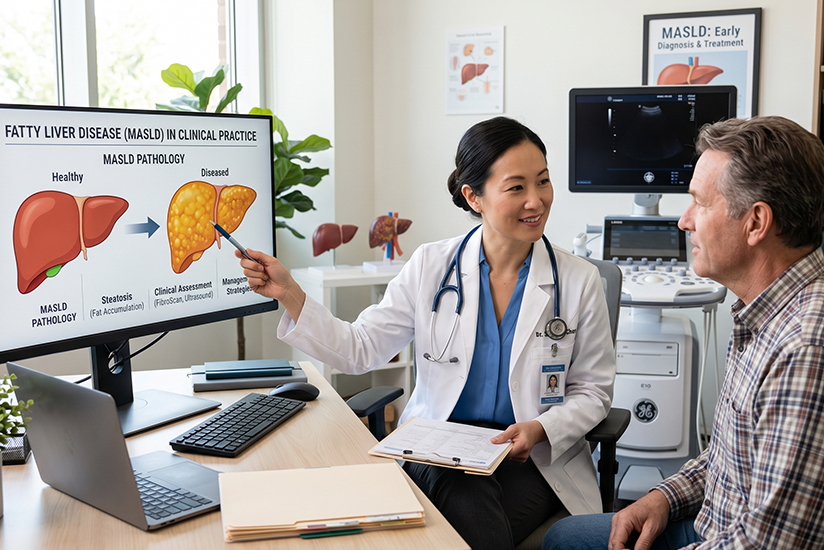
Key Points
- Prevalence rising globally and in Asia
- Strongly linked to metabolic syndrome
- Often asymptomatic
Screening Candidates
- Diabetes
- Obesity or central adiposity
- Dyslipidemia
- Hypertension
Diagnostic Tools
- ALT/AST
- Ultrasound
- FibroScan
- Non-invasive fibrosis scoring
Management
- Lifestyle modification (first-line)
- Weight loss (5–10%)
- Glycemic control
- Lipid management
Clinical Pearl
Normal BMI does not exclude fatty liver in Asians.
Localized Insight Box

Why It’s Important in the Philippines
- Rising diabetes and obesity rates
- High carbohydrate diet (rice-heavy)
- Increasing sedentary lifestyle
- Limited awareness of non-alcoholic liver disease
Public Health Opportunity
- Early screening at barangay level
- Integration into NCD programs
- Education campaigns
Final Reflection
Fatty liver disease does not begin with pain. It begins with patterns. Daily habits. Repeated choices. Quiet excess.
But the same is true for healing.
Small changes. Consistent effort. Sustained awareness.
The liver may be silent—but prevention does not have to be.











